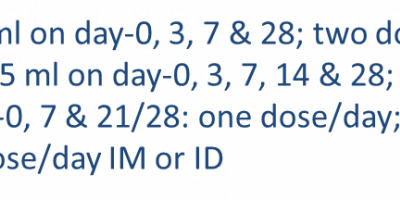Management of Animal / Dog Bite
Why is proper management of animal bite so critical?
An animal bite may potentially lead to development of Rabies and the disease is almost always fatal. Nevertheless, rabies can be prevented if timely and proper post-exposure prophylaxis (PEP) is done.