Sites to look for pallor: those surfaces of the body which have large number of superficial blood vessels with only slight natural pigments i.e.:
1. Lower palpebral conjunctiva
2. Tongue and oral mucosa
3. Nail beds
4. Palm of the hand
Looking for Pallor in the Lower Palpebral Conjunctiva:
Steps:
1. Examine in natural light.
2. Request the patient to look upwards and simultaneously pull the lower eyelid gently downward, thereby exposing the lower palpebral conjunctiva.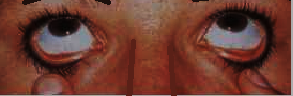
The lower conjunctiva has a half-moon shape and has been divided into:
1. Posterior rim: the posterior portion of the half-moon shape attached to the sclera
2. Anterior rim: the anterior or front portion of the half-moon shape attached to the eyelid.
Normally, the anterior rim is of bright red colour, in sharp contrast to the posterior rim which has relatively pale fleshy color.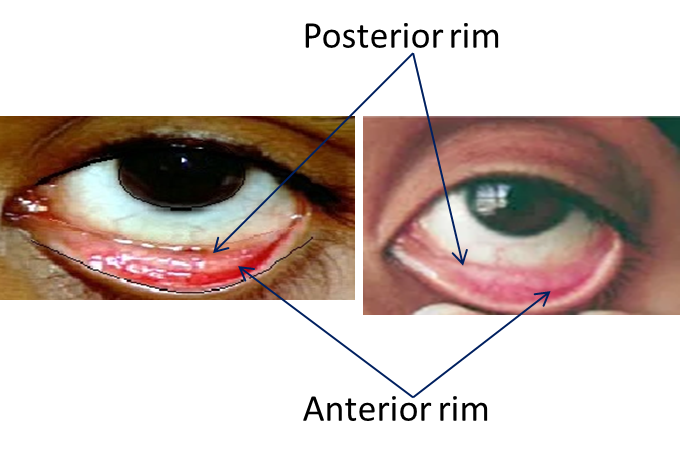
Pallor is said to be present if the anterior rim is not markedly redder as compared to the posterior rim.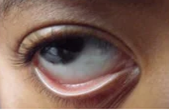
Severe pallor is considered when both, anterior and posterior rims of the palpebral conjunctiva have the same very pale fleshy color.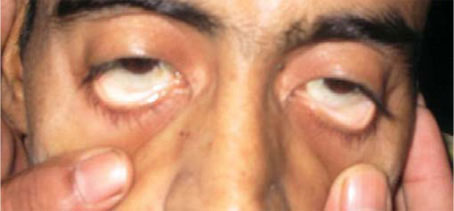
Looking for pallor in the tongue:
Ask the patient to protrude the tongue and observe the dorsal surface.
The tongue and the oral mucosa look visibly pale or severe pale.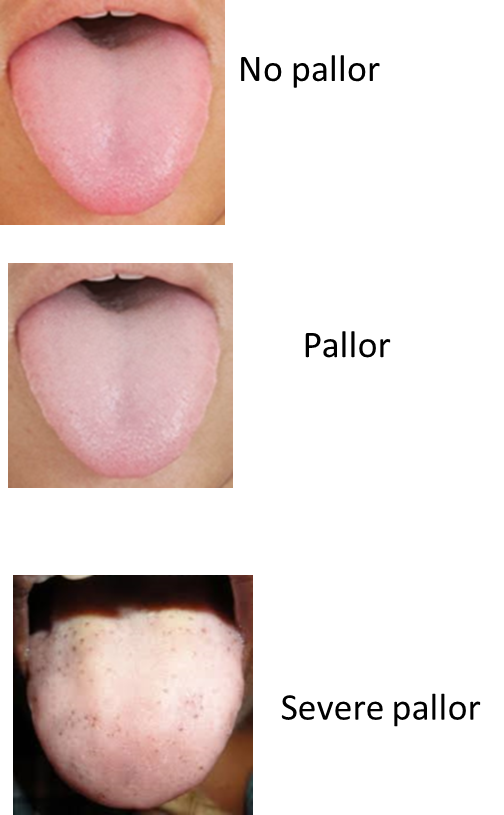
Looking for pallor in nail beds:
Inspect the nail beds and compare the colour with normal pink color of the nails of a healthy individual.
The nail beds may be pale due to reasons other than anemia also.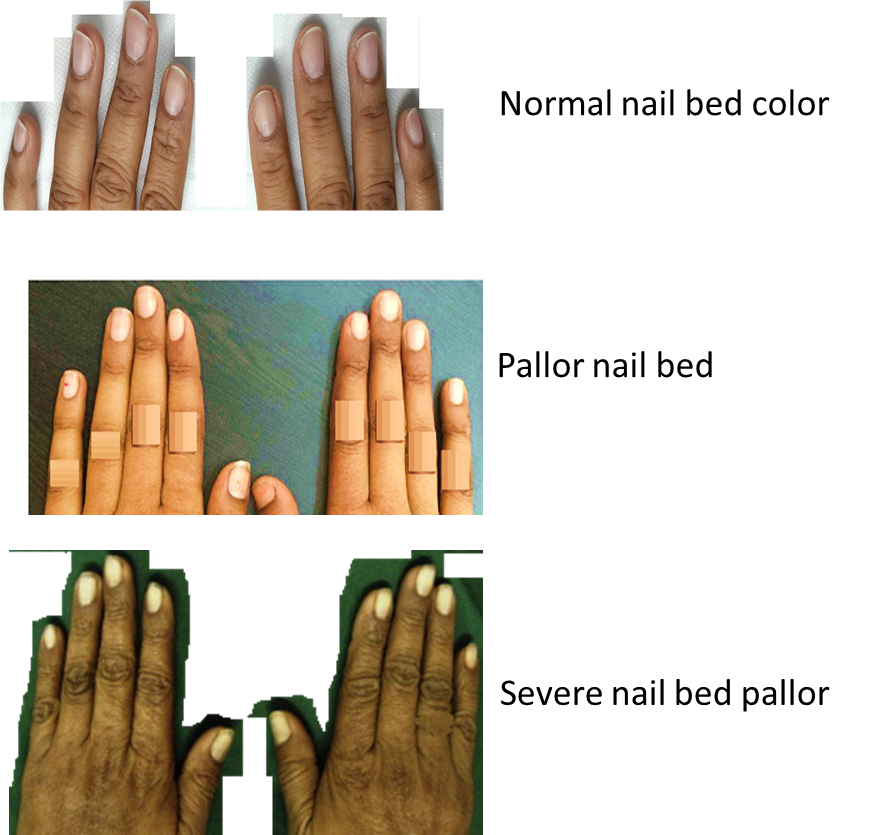
Looking for pallor in palms
Ask the patient to display the palms. Palms should not be overstretched.
Compare the pinkness of the palm with your palm or with that of a healthy person.
Next, observe for the pallor of the palmar creases. This is done by hyperextending fingers and stretching skin on either side of the creases.
If the palm is mostly pale, but the creases are darker, there is some palmar pallor. If the palm is very pale, almost white or if even the palmar creases are also pale, then severe palmar pallor is said to be present.
Assessing pallor in a child as per IMNCI guidelines:
Hold the child’s palm open by grasping it gently from the side. Do not stretch the fingers backwards.
Compare the colour of the child’s palm with your own palm and with the palms of other children.
If the skin of the child’s palm is pale, but has some pink areas, the child has some palmar pallor.
If the skin of the palm is very pale or so pale that it looks white, the child has severe palmar pallor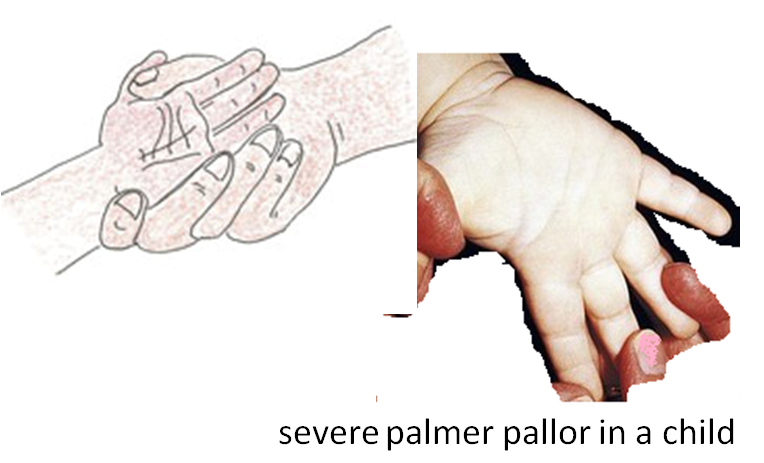
Clinical Grading of Pallor http://www.ihatepsm.com/blog/clinical-grading-pallor
Mostly, presence of pallor suggests anemia. However other phenomena may cause pallor even in absence of anemia
Eg:
• Natural skin pigmentation
• Presence of shock
• Vasoconstriction due to cold temperature
• Neural stimulation etc.
On the other hand, conjunctival pallor may be masked by conjunctival infection/inflammation and palmar pallor may be obscured by vasodilation caused by some other disorder.
References:
1. Regina D et al. Correlation of pallor with hemoglobin levels and clinical profile of anemia in primary and middle school children of rural Telangana. Int J Contemp Pediatr. 2016 Aug;3(3):872-877
2. Kalter HD, Burnham G, Kolstad PR, Hossain M, Schillinger JA, Khan NZ et al Evaluation of clinical signs to diagnose anaemia in Uganda and Bangladesh, in areas with and without malaria. Bull World Health Organ. 1997;75:103-11
3. Luby, S. P., Kazembe, P. N., Redd, S. C., Ziba, C., Nwanyanwu, O. C., Hightower, A. W., Franco, C., Chitsulo, L., Wirima, J. J., & Olivar, M. A. (1995). Using clinical signs to diagnose anaemia in African children. Bulletin of the World Health Organization, 73(4), 477–482.
4. Venkata Tulasi Ramesh Potluri, Lakshmi Spandana Potluri. Proficiency of pallor in predicting anemia. International Journal of Contemporary Medical Research 2019;6(10):J6-J9.
5. Santra G. Usefulness of examination of palmar creases for assessing severity of anemia in Indian perspective: A study from a tertiary care center. International Journal of Medicine and Public Health | Apr-Jun 2015 | Vol 5 | Issue 2
6. “Integrated management of childhood illness: conclusions. WHO Division of Child Health and Development,” Bulletin of the World Health Organization, vol. 75, supplement 1, pp. 119–128, 1997.
5-Page ANC History Taking Format: https://ihatepsm.com/blog/5-page-anc-history-taking-format-essential-gui...
Pallor and its Grading: https://ihatepsm.com/blog/pallor-and-its-grading
Why ANC History Taking Matters?: https://ihatepsm.com/blog/why-anc-history-taking-matters
#Obstetric index (GPAL) in Antenatal Case History: https://ihatepsm.com/blog/obstetric-index-gpal-antenatal-case-history
#Decoding Gravida and Para: Terms in Antenatal History Taking: https://ihatepsm.com/blog/decoding-gravida-and-para-terms-antenatal-hist...
#Duration of Pregnancy: Understanding the Trimesters and Gestational Age Categories: https://ihatepsm.com/blog/duration-pregnancy-understanding-trimesters-an...
#Calculation of Expected Date of Delivery (EDD) and Period of Gestation (POG): https://ihatepsm.com/blog/calculation-expected-date-delivery-edd-and-per...
#Antenatal Care and Case Booking: https://ihatepsm.com/blog/antenatal-care-and-case-booking
#Clinical Significance of Antenatal History Components (Socio-Demographic components): https://ihatepsm.com/blog/clinical-significance-antenatal-history-compon...
Antenatal History Taking: Significance of Clinical Components: https://ihatepsm.com/blog/antenatal-history-taking-significance-clinical...
Trimester-wise History Taking in Antenatal Care: FIRST Trimester: https://ihatepsm.com/blog/trimester-wise-history-taking-antenatal-care-f...
Trimester-wise History Taking in Antenatal Care: SECOND Trimester: https://ihatepsm.com/blog/trimester-wise-history-taking-antenatal-care-s...
Trimester-wise History Taking in Antenatal Care: THIRD Trimester: https://ihatepsm.com/blog/trimester-wise-history-taking-antenatal-care-t...
Trimester-wise History Taking in Antenatal Care: A Comprehensive Guide (all 3 trimesters): https://ihatepsm.com/blog/trimester-wise-history-taking-antenatal-care-c...
Components of Birth Preparedness and Complication Readiness (BPCR): https://ihatepsm.com/blog/components-birth-preparedness-and-complication...
BPCR in brief: https://ihatepsm.com/blog/%E2%80%98birth-preparedness-and-complication-r...
Specific Health Protection during Antenatal Visits: https://ihatepsm.com/blog/specific-health-protection-during-antenatal-vi...
